On all honey jars, raw or commercially processed (found in supermarkets), we read this warning: “Not suitable for children under 1 year old.” If honey is that good, why can’t you give honey to infants, too?
As unbelievable as it may sound, honey may become dangerous to an infant. This means it may be potentially toxic.
So, what do we do, we refrain from giving them honey?
This is a good option. Though modern technology offers us another alternative: medical grade honey, which is sterile and has a minimum composition change.
Why does honey need sterilization?
Because their digestive system is still developing. Honey may contain spores of a bacterium called clostridium botulinum. We say spores, but they are actually endospores, which are egg-like bacteria in conservation form.
What are endospores?
Lack of nutrients make certain bacteria reduce themselves to this form, a dormant, tough, and non-reproductive structure. Insides these endospores bacteria lie dormant for extended periods, even centuries. (There are many reports of spores remaining viable over 10,000 years, and revival of spores millions of years old has been claimed.)
These endospores can be present in food, honey included.
Why would a mother give honey her baby?
To sweeten the food, even the milk if he/her doesn’t like it as it is.
Or, from medical reasons, to help him/her grow better.
What is botulism?
Botulism is a rare and potentially fatal illness caused by a toxin (botulinum toxin) produced by the bacterium Clostridium botulinum. This bacterium is a a large anaerobic Gram-positive bacillus, a soil bacterium that forms subterminal endospores.
In anaerobic conditions (low oxygen levels and certain temperatures) the bacterium produces the toxin, which produces the following symptoms in humans: the motor nerve endings are prevented from releasing acetylcholine, causing flaccid paralysis and symptoms of blurred vision, ptosis, nausea, vomiting, diarrhea or constipation, cramps, and respiratory difficulty. The disease does not usually affect consciousness or cause a fever. Death occurs in 5 to 10% of people.
Treatment is with an antitoxin and supportive care.
Why are only babies affected by botulinum spores?
This is not true. Though it is common only to babies, due to their undeveloped digestive system, there are cases of botulism in adults.
1. In adults botulism poisoning can occur due to preserved or home-canned, low-acid food that was not processed using correct preservation times and/or pressure. This poisoning is called Foodborne botulism.
Signs and symptoms usually begin between 18 and 36 hours after the toxin gets into your body, but can range from a few hours to several days, depending on the amount of toxin ingested.
Among the symptoms: double vision, blurred vision, drooping eyelid, nausea, vomiting, and abdominal cramps and so on.
2. Other cases appear among those who inject street drugs. The illness is known as wound botulism. In this situation, spores enter a wound, and in the absence of oxygen, release the toxin. It is not passed directly between people.
It is common in people who inject black tar heroin. The symptoms include: Difficulty swallowing or speaking, Facial weakness on both sides of the face, blurred or double vision, drooping eyelids, trouble breathing, paralysis.
3. A very rare form of botulism, known as adult intestinal toxemia, may occur by the same route as infant botulism but is among adults. Occurs rarely and sporadically.
Infant boltulism
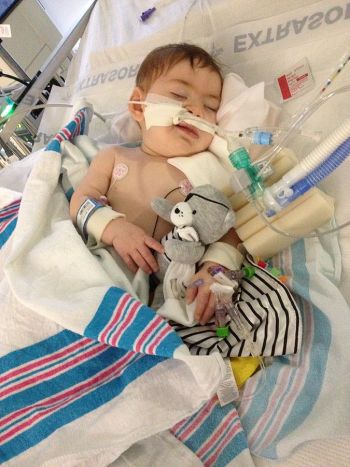
Infant botulism, also known as floppy baby syndrome, is the most common form of botulism in the United States and was first recognized in 1976.
The term “floppy infant syndrome” is used to describe abnormal limpness when an infant is born.
After ingestion of the Clostridium botulinum endospores, the colonization of the small intestine takes place.
This happens because the composition of the intestinal microflora (normal flora) is insufficient to competitively inhibit the growth of Clostridium botulinum and levels of bile acids (which normally inhibit clostridial growth) are lower than they will be later in life.
This typically only occurs in children less than six months old (more than 90% of cases), as their protective mechanisms develop after that time.
As soon as infants begin eating solid food, the digestive juices become too acidic for the bacterium to grow.
The bacterium releases botulinum toxin, which is then absorbed into the bloodstream and taken throughout the body, causing paralysis by blocking the release of acetylcholine at the neuromuscular junction.
What are the symptoms of infant botulinum
Typical symptoms of infant botulism include constipation, lethargy, weakness, difficulty feeding and an altered cry, often progressing to a complete descending flaccid paralysis. Although constipation is usually the first symptom of infant botulism, it is commonly overlooked.
Is honey the true cause of botulism?
Honey is blamed everywhere for containing these spores, and for this reason, it is not recommended for infants younger than 12 months old.
However, most cases of infant botulism are thought to be caused by acquiring the spores from the natural environment. Clostridium botulinum is a ubiquitous soil-dwelling bacterium.
Many infant botulism patients have been demonstrated to live near a construction site or an area of soil disturbance.
Infant botulism has been reported in 49 of 50 US states, and cases have been recognized in 26 countries on five continents.
Can we fight against infant botulism?
To prevent foodborne botulism we need to take some preventive cooking measures.
The toxin, though not the bacterium, is destroyed by heating it the food to more than 85 °C (185 °F) for longer than 5 minutes. other scientists say “all types of botulinum toxin are rapidly destroyed by heating to 100 °C for 15 minutes”. Honey does not contain the toxin, but the endospores which contain the bacterium, and for this reason, heating honey will not kill it. It may still be contained in the commercial honey found on the shelves, on which producers used only heat for filtration or pasteurization.
Growth of the bacterium can be prevented by high acidity, high ratio of dissolved sugar, high levels of oxygen, very low levels of moisture, or storage at temperatures below 3 °C (38 °F) for type A.
For example, in a low-acid, canned vegetable such as green beans that are not heated enough to kill the spores may provide an oxygen-free medium for the spores to grow and produce the toxin. However, pickles are sufficiently acidic to prevent growth; even if the spores are present, they pose no danger to the consumer.
When can we give honey to babies?
To prevent infant botulism we simply should not give honey to our infants. However, if you manage to find one, give the, honey sterilized using the gamma-irradiation method. It’s a safe honey that still preserves all its health benefits. Read this article to understand why: Gamma irradiated honey is safer than raw honey and with the same antibacterial power!
Can infant botulism be treated?
Yes, with the antitoxin and lots of medical care. There are no long-term side effects, but can the illness may be complicated by hospital-acquired infections.
Death may occur due to respiratory failure. Mechanical ventilation (breathing support through a ventilator) as well as intensive medical and nursing care, are required and sometimes for several months! And after leaving the hospital, rehabilitation therapy may be required.
However, in the past 50 years, the proportion of patients with botulism who die has fallen from about 50% to 7% due to improved supportive care.
Botulinum toxin is good for something!
Scientists have found a method of treating some illnesses using diluted purified botulinum toxin.
There have bee beneficial effects in treating: congenital pelvic tilt, spasmodic dysphasia (the inability of the muscles of the larynx), achalasia (esophageal stricture), strabismus (crossed eyes), paralysis of the facial muscles, failure of the cervix, blinking frequently or as anti-cancer drug delivery.
C. botulinum is also used to prepare the drugs Botox, Dysport, Xeomin, and Neurobloc used to selectively paralyze muscles to temporarily relieve muscle function. It has other “off-label” medical purposes, such as treating severe facial pain, such as that caused by trigeminal neuralgia.
===================
References:
https://en.wikipedia.org/wiki/Botulism#Infant_botulism
https://en.wikipedia.org/wiki/Clostridium_botulinum
A photomicrograph of Clostridium botulinum bacteria” picture – By Content Providers: CDC – This media comes from the Centers for Disease Control and Prevention’s Public Health Image Library (PHIL), with identification number #2107.Note: Not all PHIL images are public domain; be sure to check copyright status and credit authors and content providers.English | Slovenščina | +/−, Public Domain, https://commons.wikimedia.org/w/index.php?curid=68204



